Originally published by The 19th.
As more abortion bans have gone into effect across the country, it has become far more difficult to perform a standard element of gynecological care: screening patients for domestic abuse.
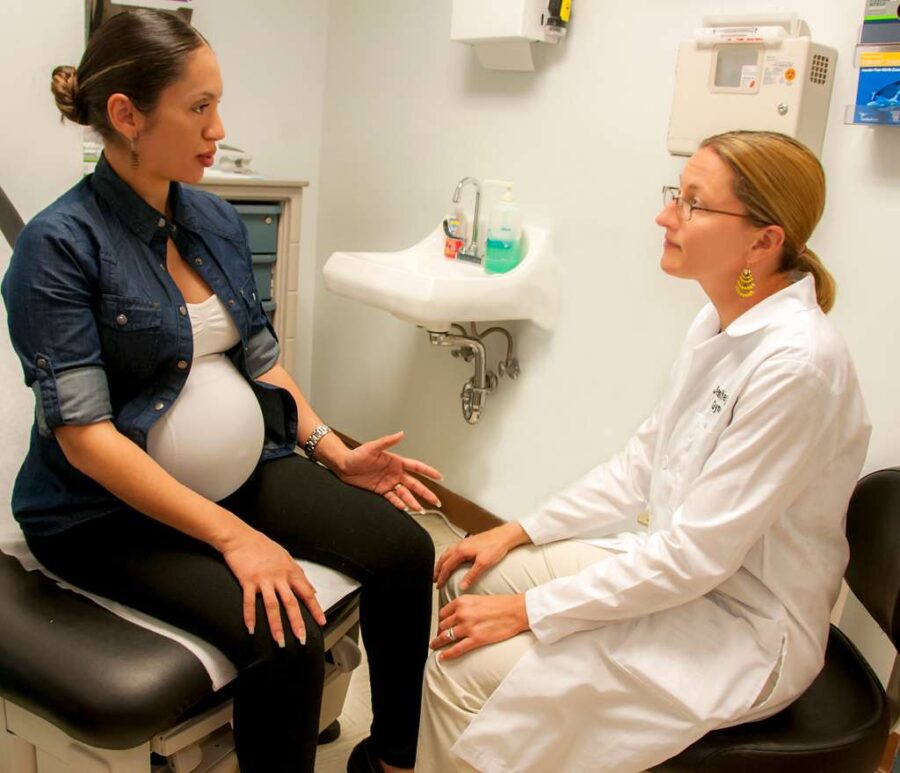
As OB-GYNs leave states with abortion bans, with them goes the first line of defense for women facing domestic violence
Originally published by The 19th.
As more abortion bans have gone into effect across the country, it has become far more difficult to perform a standard element of gynecological care: screening patients for domestic abuse.

Research shows that OB-GYNs are often the first or only doctors to learn if a patient is facing intimate partner violence. While women of all ages experience intimate partner violence, it is most prevalent among women of reproductive age, the people most likely to see an OB-GYN. Meanwhile, abortion bans have contributed to reproductive health care providers leaving states, retiring early or declining to practice where the procedure is restricted.
There is little data on the trend, but doctors and experts agree that as a result, people experiencing domestic violence are less likely to be appropriately screened—let alone connected to resources or support.
The impact is particularly visible in Idaho. Reproductive health specialists were already in short supply in the state before Roe v. Wade fell. And the majority of maternal-fetal medicine physicians—doctors who specialize in complex pregnancies—have left the state over the past year, explicitly linking their departure to the state’s punitive abortion law, which treats provision of abortion as a felony, only allows the procedure if it is necessary to save a patient’s life, and still requires physicians to defend themselves in court for providing such care.
So the number of providers who are screening for intimate partner violence is dwindling. And those who remain in the state will be forced to take on larger patient loads, leaving less time for such complex conversations, some physicians fear.
“We’re creating conditions in this state where it’s going to be more and more difficult for someone to come forward for help,” says Kelly Miller of the Idaho Coalition Against Sexual and Domestic Violence.
As Miller explained, the ban has created additional stress on parts of the state that already face barriers to abortion care because of the way they are surrounded by other states with limited access and restrictive laws.
While western Idaho affords proximity to Oregon and Washington state, where abortion is protected and more readily available, the northern part of the state contains many tribal lands that already experience barriers to health care generally. Southern Idaho borders Utah, Wyoming and Montana, states that also have abortion restrictions. As a result, depending on where someone lives, access to reproductive health care—and thus screening for intimate partner violence—can be “more dire.”
Health care systems, researchers and domestic violence experts have been pushing for years to expand the role medical providers play in screening for and addressing intimate partner violence, which research suggests affects 1 in 3 women. Transgender and nonbinary people also face staggering rates of domestic and intimate partner violence: Per the most recent U.S. Transgender Survey in 2015, 54% of all respondents said they experienced some form of intimate partner violence, including physical violence and preproductive coercion—any way in which a partner might attempt to exercise control over the other’s reproductive health.
The federal government recommends that physicians screen women for signs that they may be experiencing violence at home, as does the American College of Obstetricians and Gynecologists (ACOG). In their guidance, ACOG also acknowledges that intimate partner violence is experienced by both men and women of all sexual orientations.
OB-GYNs and other reproductive health care professionals can play an outsized role in screening for intimate partner violence. ACOG advises using doctors’ visits for a private conversation about patients’ safety at home and in their relationships and, if needed, connecting patients with resources and support, including contraception, abortion or safety planning.
There is research showing patients are more likely to disclose personal information with their OB-GYNs; a poll from 2017 found that 61% of women were more likely to be honest with those medical providers than with a general practitioner. In their guidance, ACOG cites the unique nature of the physician-patient relationship within the context of reproductive health care as a critical reason why these providers should screen for intimate partner violence.
Doctors told The 19th there is a particular intimacy between a patient and OB-GYN. OB-GYNs are also often the health care providers that women most often see for routine medical care, making the exam room an effective place to assess their risk of experiencing violence. According to ACOG, approximately 324,000 pregnant women are abused by intimate partners each year, and intimate partner violence is associated with adverse fetal outcomes. Research has shown that the severity of violence in an intimate partner setting is known to escalate during pregnancy.
“We very much value privacy and the sanctity of the visit and the exam room. Most people feel safe once they’re here and the door is closed to be able to share information with us,” says Dr. Rebecca Uranga, an OB-GYN in Meridian, Idaho. “It’s just by nature of what we do and how we’re trained. That’s our culture.”
Uranga, who comes across a patient maybe once a year who is experiencing domestic violence, is part of an initiative to expand and improve upon how reproductive health providers talk to patients about the issue. But the exodus of medical providers in Idaho is undercutting those efforts. Multiple physicians said it has grown harder to recruit not only OB-GYNs and maternal-fetal medicine specialists, but also family doctors, in large part because of the state’s abortion ban. Uranga fears that soon there won’t be enough doctors to simply ask patients if they are safe at home.
“Who will be asking is going to get smaller,” she says. “Someone needs to be asking.”
Caring for people who experience intimate partner violence is particularly complex, said Dr. Ashley King, a family medicine provider in Boise who also works specifically with survivors of domestic violence. Despite efforts to expand health care’s role in screening for and addressing violence, not all doctors are comfortable providing such care—meaning that every physician departure strains an already small pool.
“If we continue to make more and more restrictive laws that discourage providers from coming to Idaho in the first place, we will have a significant problem with shortage of access to health care across the board—let alone for those people to have the time and bandwidth to do the work like screening for intimate partner violence,” she said.
The current situation in Idaho is “incredibly worrisome,” Miller says. Research shows that homicide as a result of domestic violence is the largest single cause of death for pregnant and recently postpartum Americans. The presence of guns, which are in 60% of Idaho households, heightens the risk.
Because the state’s laws threaten criminal penalties for abortion and helping someone to access abortion, doctors and sexual and domestic violence program advocates alike are under an acute pressure that has left even non-clinical program workers in social support network programs afraid to help survivors, especially if their work could be construed as having connected pregnant survivors of violence to abortion services, Miller said.
Though concerns for intimate partner violence screening are particularly visible in Idaho, clinicians said that barriers to care have emerged across the country as abortion bans proliferate. So far, 14 states have almost-completely banned the procedure, and seven more have imposed gestational limits before viability, the point at which a fetus can live independently outside the uterus.
The impact is visible at the Washington, D.C.-based DuPont Clinic, one of the few providers to offer abortions through all trimesters of pregnancy and a national destination for people seeking abortions later in pregnancy.
While the clinic has always seen patients who have traveled to D.C. for care, the share of such patients has only increased over the past year, says Elizabeth Bastias-Butler, DuPont’s director of clinical services. Before patients arrive at DuPont, clinicians perform an intimate partner violence screen as part of their intake process, as well as a safety screen with each patient when they arrive in person at the clinic. Since more abortion bans have taken effect post-Dobbs nationwide, Bastias-Butler says the clinic now sees more patients also experiencing intimate partner violence.
Many patients do not disclose over the phone during their intake screen that they are unsafe at home and in need of help, Bastias-Butler says. “Sometimes, they’ve never told anyone what their experiences are until they are in clinic with us when we do our intake,” she says. The in-person visit is often the very first time a person feels comfortable disclosing that they are experiencing domestic violence.
“We have definitely had instances in which we have had to secure different modes of transportation home for a patient who has actually come to the clinic with a partner,” Bastias-Butler says.
Bastias-Butler adds that oftentimes, people assume that someone who is experiencing intimate partner violence is terminating a pregnancy as a means of getting away from a partner, to create a situation where there are fewer ties to someone who is hurting them. In reality, she says, many of the patients they see who are experiencing domestic violence come to DuPont Clinic because of fatal fetal abnormalities or risks a pregnancy poses to their own health. These patients often find that coming for this form of care and building trust with a provider allows them to then disclose the violence they are experiencing at home—and ask for help.
If and as more bans take effect, the implications for domestic violence survivors will spread, said Dr. Carrie Rouse, a maternal-fetal medicine physician at Indiana University. Her state—where reproductive health specialists were already hard to come by—has also seen a drop-off in applications from aspiring medical residents, a change she attributes to its recently enforced abortion ban. With fewer physicians, she said, patients here too will have to drive travel appropriate and adequate Ob-Gyn care, including baseline screening for domestic violence.
“It’s scary to think about,” she says. “We know that many people who are in a situation of intimate partner violence don’t seek help when they’re asked the first time. It often takes multiple attempts, multiple offers of help. By decreasing the number of interactions and access, we are effectively decreasing the chance that someone gets help when they need it.”

Jennifer Gerson was the recipient of the 2015 Maggie Award for her reproductive and sexual health reporting work at Yahoo Health. In 2019, she was twice nominated by the American Society of Magazine Editors for her work in Marie Claire and Cosmopolitan. She was also one of the founding editors of Jezebel.com.

Shefali Luthra covers the intersection of gender and health care. She is a former correspondent at Kaiser Health News, where she spent six years covering national health care and policy.
Have thoughts or reactions to this or any other piece that you’d like to share? Send us a note with the Letter to the Editor form.
Want to republish this story? Check out our guide.

